What do proteins have to do with COVID-19 research? The answer: everything. In the battle against the COVID-19 infection, the spike protein of pathogen SARS-CoV-2 is the main point of interest. The spike protein is a structural part of the shell that protects the viral genome and could be the key for medicaments and vaccines. An overview of what is currently being done in research and what role ACE2, TMPRSSE, camostat mesylate or the CR3022 antibody play is explained in the following article.
About COVID-19
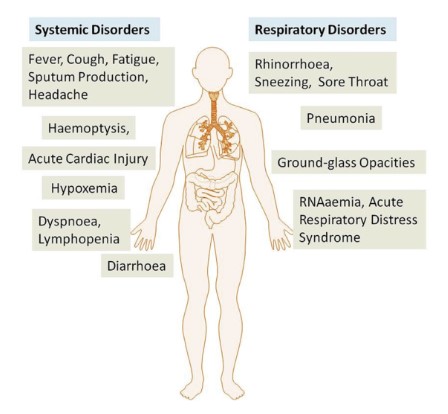
In late 2019, several cases of pneumonia of unknown origin were reported. Since then, COVID-19 has been spreading around the world and declared as a pandemic by the World Health Organization (WHO) in March 2020. COVID-19 includes among other symptoms cough, difficulty breathing and fever, and can be severe even lead to death.
Why it is called coronavirus
The name of the coronavirus comes from the Latin word “corona”, which means crown. When observing the virus under the electron microscope, coronaviruses appear surrounded a crown-like structure. This is due to the presence of viral spike proteins characterizing a spherical morphology.
About SARS-COV-2
SARS-CoV-2 is a novel beta coronavirus is less pathogenic than SARS-CoV or MERS virus but higher transmissibility from human to human. SARS-CoV and SARS-CoV-2 are very similar in structure, but the most important structure protein is slightly different: the spike protein. Coronavirus are ~30 kilobase positive-sense RNA viruses and they consist of a nucleocapsid surrounded by an envelope which contains three structural proteins: (S) spike, (M) membrane and (E) envelope, as well as multiple non-structural proteins. The viral genome is protected within the nucleocapsid.
Research on SARS CoV-2
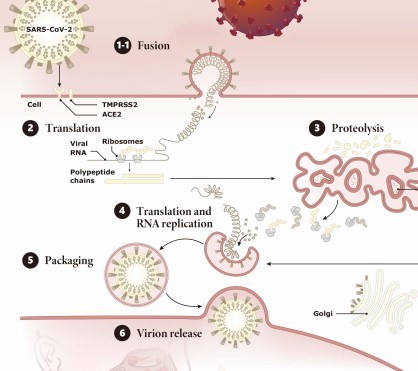 The rapid spread of COVID-19 has resulted in an urgent start of the research to find therapeutic strategies against SARS-CoV-2. Major focus of this research is on the virus spike protein, which with the S1 subunit of the RBD mediates the viral binding and membrane fusion through interaction with the angiotensin converting enzyme 2 (ACE-2) receptor on the host cell. Targeting this interaction between ACE2 and S protein could be a potential approach.
The rapid spread of COVID-19 has resulted in an urgent start of the research to find therapeutic strategies against SARS-CoV-2. Major focus of this research is on the virus spike protein, which with the S1 subunit of the RBD mediates the viral binding and membrane fusion through interaction with the angiotensin converting enzyme 2 (ACE-2) receptor on the host cell. Targeting this interaction between ACE2 and S protein could be a potential approach.
Another way to stop the entering of the virus could be targeting the serine protease TMPRSS2 which is necessary for the priming of the spike protein needed in the entry into host cells. Camostat mesylate inhibits TMPRSS2, this could significantly reduce lung cell infection with SARS-CoV-2 and could be considered for COVID-19 treatment.
During COVID-19 infection, the inflammatory response can be strong causing a cytokine storm.
It is important to fully understand the role these proteins play in SARS-CoV-2 infection. Varieties of antibodies as well as proteins are needed to investigate the mechanisms of the SARS-CoV-2 life cycle.
The monoclonal antibody CR3022 was originally obtained from a convalescent SARS-CoV patient, binds to a highly conserved site in the RDB, leading to destabilization of the prefusion spike conformation. The CR3022 antibody could be potentially used as a COVID-19 therapeutic.
Yale University developed a saliva-based COVID-19 test where Proteinase K is added to the saliva, heated up to 95 °C during 5 min and used directly for RT-qPCR without any RNA extraction. This is a faster and cheaper method for SARS-CoV-2 detection.
In addition, there also exist antigen and antibody rapid test to detect in a few minutes if a patient suffers from COVID-19 or has developed antibodies after the infection.

 Deutsch
Deutsch


